
Imagine walking into a room where every step sends sharp pain shooting through your big toe. You know the feeling. It’s not just an occasional ache; it’s a relentless reminder that something is wrong with how your body handles uric acid, a waste product formed when the body breaks down purines found in certain foods and drinks. For millions of people living with gout, a form of inflammatory arthritis caused by high levels of uric acid in the blood leading to crystal formation in joints, the old advice of "just take painkillers when it hurts" no longer cuts it. We’ve moved past treating symptoms alone. Today, we talk about controlling the disease at its source.
The game-changer? A strategy called treat-to-target therapy, a clinical approach where medication doses are adjusted based on specific laboratory results rather than symptom presence alone. This isn’t guesswork. It’s precision medicine. By keeping your serum urate levels below a specific threshold, you stop new crystals from forming and dissolve the old ones hiding in your joints. The question isn't whether this works-it does-but how you get there using medications like allopurinol, the most commonly prescribed xanthine oxidase inhibitor for lowering uric acid production or febuxostat, a non-purine selective xanthine oxidase inhibitor used as an alternative for patients who cannot tolerate allopurinol.
What Are the Exact Urate Targets?
Let’s cut through the confusion. If you’re asking what number you should aim for on your lab report, the answer is straightforward but requires nuance depending on your severity. Major guidelines, including those from the American College of Rheumatology (ACR) and NICE, agree on one core principle: lower is better, up to a point.
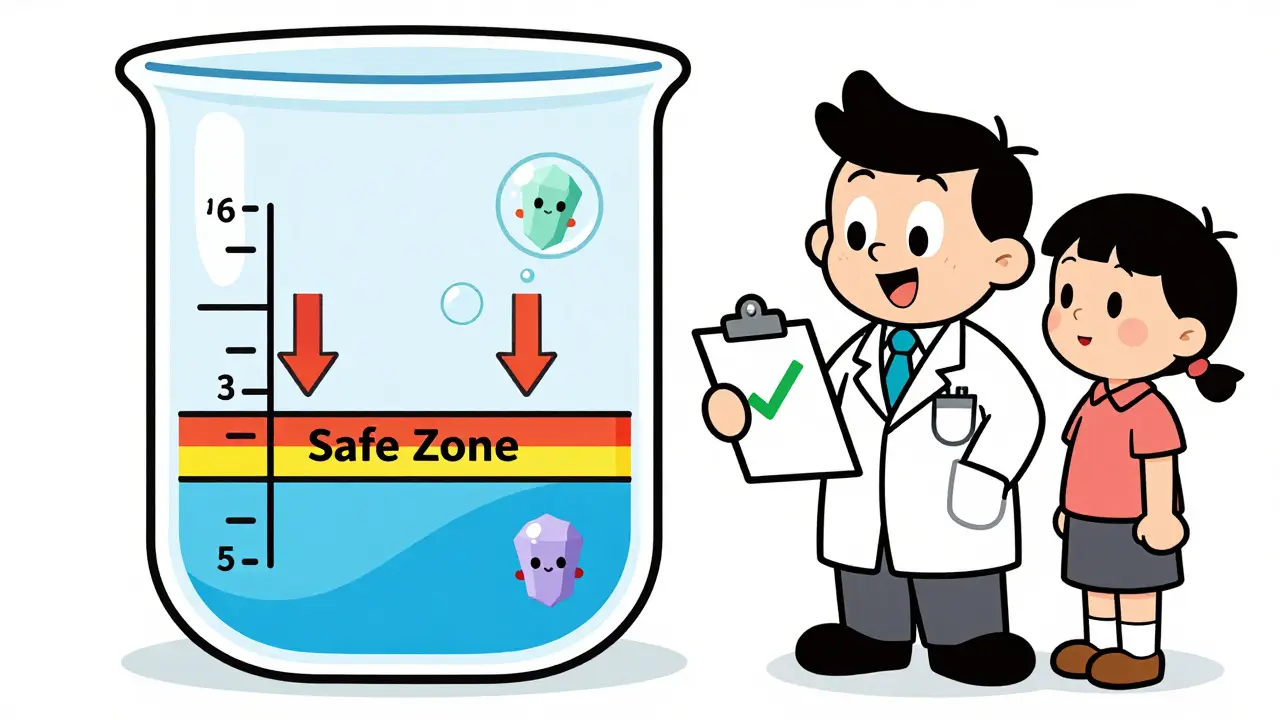
For most patients starting urate-lowering therapy (ULT), the target is a serum urate level of less than 6 mg/dL (360 micromol/L). Think of 6.8 mg/dL as the saturation point-the temperature at which water turns to ice. Above this level, uric acid crystallizes. Below it, crystals begin to dissolve. However, if you have severe gout-characterized by visible lumps under the skin known as tophi, collections of monosodium urate crystals that form under the skin in chronic gout cases, joint damage seen on X-rays, or frequent flares despite treatment-you need to go lower. In these cases, the target drops to less than 5 mg/dL (300 micromol/L).
Here is the critical boundary: do not let your levels drop below 3 mg/dL (180 micromol/L). There is no proven benefit to going lower than this, and potential risks increase without clear reward. Your goal is to stay safely between 3 and 6 mg/dL, or 3 and 5 mg/dL if your case is severe. This isn’t a suggestion; it’s the foundation of modern gout management.
| Patient Profile | Target Serum Urate Level | Rationale |
|---|---|---|
| Standard Gout | < 6 mg/dL (< 360 µmol/L) | Prevents crystal formation and promotes dissolution in typical cases |
| Severe Gout (Tophi, Joint Damage) | < 5 mg/dL (< 300 µmol/L) | Accelerates tophus resolution and prevents further structural damage |
| Lower Limit Warning | Not < 3 mg/dL | No additional benefit; potential unknown risks |
Allopurinol: The First-Line Workhorse
When doctors prescribe ULT, allopurinol is almost always the first choice. Why? Because it works, it’s affordable, and decades of data support its safety profile when used correctly. It belongs to a class of drugs called xanthine oxidase inhibitors, which block the enzyme responsible for producing uric acid.
The biggest mistake patients make? Starting too high. You might think, "If I’m in pain, I need a strong dose." But with allopurinol, slow is smooth, and smooth is fast. Guidelines recommend starting at a low dose-typically 100 mg per day, or even 50 mg if you have moderate to severe kidney disease (CKD stage 3 or higher). From there, you titrate up gradually. Every 2 to 4 weeks, check your serum urate. If you haven’t hit your target, increase the dose by 50 to 100 mg.
Many patients don’t realize they need more than the standard 300 mg daily dose. Real-world data from New Zealand shows that 30-50% of patients require doses exceeding 300 mg to reach their targets. In fact, doses up to 600-800 mg/day can be safe and effective for patients with normal kidney function, helping 75-80% of them achieve control. Don’t stop at 300 mg just because it’s the "standard" pill size. Keep going until your blood work says you’ve won.
Febuxostat: When Allopurinol Isn’t Enough
So, when do you switch to febuxostat? This drug works similarly to allopurinol by inhibiting xanthine oxidase, but it has a different chemical structure. It’s often considered when:
- You experience a hypersensitivity reaction to allopurinol.
- You have severe chronic kidney disease (CKD) where allopurinol dosing becomes tricky.
- You fail to reach targets despite maximum tolerated doses of allopurinol.
Febuxostat starts at 40 mg daily and can be increased to 80 mg if needed. Some studies suggest it may be slightly more effective in achieving targets in patients with severe CKD, showing a 15% higher success rate in some meta-analyses. However, cost is a factor. Generic allopurinol costs roughly $4-$12 per month, while febuxostat can run $30-$50. Insurance coverage varies, so discuss this openly with your provider.
There is also a cautionary note. The FDA issued a boxed warning for febuxostat regarding cardiovascular risk compared to allopurinol. While subsequent studies have nuanced this finding, it remains a consideration for patients with existing heart conditions. Always weigh efficacy against personal health history.
The "Flare Paradox": Why It Gets Worse Before It Gets Better
Here’s where many patients quit. You start your medication, your uric acid drops, and suddenly-boom-another flare. It feels counterintuitive. Why would lowering the cause of the problem trigger the problem itself?
This is known as the "flare paradox." As your serum urate levels drop rapidly, existing crystals in your joints begin to destabilize and shed. Your immune system sees these shifting crystals as invaders and launches an inflammatory attack. It’s a sign that the medicine is working, but it’s painful.
To prevent this, you must use prophylaxis. Doctors typically prescribe colchicine or a low-dose NSAID alongside your ULT for the first 3 to 6 months. Do not skip this step. Taking anti-inflammatory protection allows you to titrate your allopurinol or febuxostat upward without triggering constant attacks. Once your levels stabilize below target for several months, the flares usually stop entirely.
Monitoring and Titration: The Key to Success
Treat-to-target is not a set-it-and-forget-it strategy. It requires active monitoring. How often should you test? Monthly during the titration phase. Yes, monthly. Waiting three or six months between tests slows progress significantly. Data shows that monthly monitoring increases target achievement by 31% compared to quarterly checks.
Keep a simple log:
- Date: When you took the blood test.
- Serum Urate Level: The actual number.
- Current Dose: What you were taking.
- Action: Did you increase, decrease, or maintain?
If you miss your target after two consecutive tests spaced 30 days apart, it’s time to adjust. If you hit it, hold steady for a few months to ensure stability. Remember, consistency matters more than speed. A gradual rise in dosage reduces side effects and improves long-term adherence.

Barriers to Reaching Target
Despite clear guidelines, only about 42% of patients achieve their target within 12 months. Why? Several barriers exist:
Lack of Provider Education: Many primary care physicians still view gout as a dietary issue rather than a metabolic disorder requiring strict biochemical control. They may initiate ULT but fail to titrate aggressively enough.
Patient Fear of Side Effects: Concerns about allopurinol hypersensitivity syndrome (AHS) are valid but rare (0.1-0.4% of patients). Genetic testing for HLA-B*5801 can identify those at highest risk, particularly in Asian populations, allowing for safer prescribing.
Systemic Inequities: Studies show disparities in care. For example, Māori and Pacific populations in New Zealand have higher dispensing rates but lower target achievement due to access barriers. Advocating for yourself and seeking rheumatologist support can bridge this gap.
Future Directions and Precision Medicine
We are entering an era of personalized gout care. Emerging research looks at genetic markers like ABCG2 and SLC22A12 polymorphisms to predict how well you’ll respond to allopurinol. Early trials suggest genotype-guided dosing could boost target achievement from 61% to 83%. Additionally, new uricosurics like verinurad are in development, offering alternative mechanisms for patients who struggle with xanthine oxidase inhibitors.
Until then, stick to the basics. Know your numbers. Take your meds consistently. Monitor monthly. And remember: gout is curable. Not manageable. Curable. With the right strategy, you can dissolve those crystals and walk pain-free again.
What is the ideal serum urate level for gout patients?
The general target is less than 6 mg/dL (360 micromol/L). For patients with severe gout, tophi, or joint damage, the target is stricter: less than 5 mg/dL (300 micromol/L). Levels should never fall below 3 mg/dL.
Should I start with allopurinol or febuxostat?
Allopurinol is the recommended first-line treatment for most patients due to its efficacy, safety profile, and low cost. Febuxostat is reserved for those who cannot tolerate allopurinol, have severe kidney disease, or fail to reach targets with allopurinol.
Why do I get more flares when I start medication?
This is the "flare paradox." Rapid changes in uric acid levels cause existing crystals to shift and break apart, triggering inflammation. Taking prophylactic anti-inflammatory drugs like colchicine for the first 3-6 months helps prevent this.
How often should I check my serum urate levels?
During the initial titration phase, you should test monthly. This allows for timely dose adjustments. Once you reach your target, testing frequency can decrease to every 6-12 months to monitor maintenance.
Can I stop taking ULT once my levels are normal?
No. Urate-lowering therapy is typically lifelong. Stopping the medication will cause uric acid levels to rise again, leading to crystal reformation and future flares. Consistent maintenance is key to preventing disease progression.





Categories